GUM DISEASE
What is gum disease
Periodontitis, also known as gum disease, is a preventable infection that can lead to tooth damage and loss. It starts with the buildup of plaque and tartar caused by oral bacteria. Indications of gum disease include bleeding, receding, and swollen gums, as well as tooth loss. Fortunately, gum disease can be treated and detected by a dentist, even in its early stages. If left untreated, it can result in serious health issues like the risk of stroke and heart attack.
Gum disease can be categorized into three stages with varying levels of severity: gingivitis, periodontitis, and advanced periodontitis. During the gingivitis stage, inflammation causes the pockets formed by the gums around the teeth to enlarge. The dentist can measure the space between the teeth and gums to assess the extent of damage. If this space measures more than three millimeters, it indicates a potential for further complications.
As gingivitis progresses to periodontitis, prolonged exposure to plaque and tartar increases the space between the gums and teeth. At this stage, bone loss begins and the gums easily bleed.
In the final stage, advanced periodontitis, significant bone loss may occur. The gap between the teeth and gums allows bacteria to reach the socket and roots of the teeth. This bacterial presence weakens the tooth’s attachment to the bone, making immediate treatment crucial to prevent tooth loss.
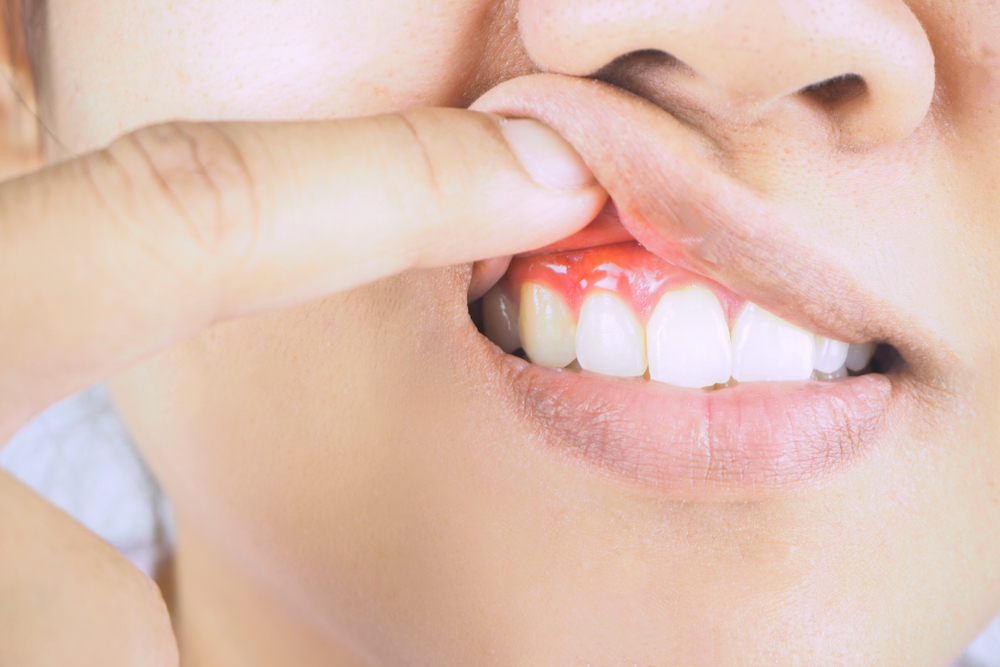
Gum Disease treatment
Treatment for early-stage gum disease may involve more frequent dental cleanings to remove tartar before it causes significant harm. As gum disease advances, dental scaling becomes necessary to eliminate plaque and tartar that have penetrated deeper beneath the gums. These deeper cleanings should feel no different from regular cleanings when anesthetic is used. In certain situations, a tooth whitening tray-like device may be employed to facilitate medication penetration into the deeper gum areas. In cases of severe gum disease, laser therapy or oral surgery might be required to address bacterial damage and treat receding gums.